In today’s rapidly evolving healthcare landscape, technology is both an enabler and a game-changer. Healthcare software, in particular, has emerged as a vital component in the industry’s quest for efficiency, quality patient care, and streamlined processes.
For patients, healthcare professionals, administrators, and organizations, understanding the role and impact of healthcare software is paramount to staying competitive and ensuring the delivery of high-quality care.
Would you like to learn the best kept secrets to using healthcare software to optimize healthcare delivery? This article is a comprehensive guide for mainly patients and all healthcare workers on the significance of healthcare software and how to implement it to improve overall health. You’ll also learn about options to acquire and access relevant healthcare software for maximum impact.
Have an innovative healthcare software idea? Need help developing it? At Iterators we can help design, build, and maintain custom software solutions for both startups and enterprise businesses.
Schedule a free consultation with Iterators today. We’d be happy to help you find the right software solution to help your company.
What is Healthcare Software
At its core, healthcare software encompasses a diverse range of applications, platforms, and systems designed to streamline and optimize healthcare processes, from patient management to data analysis.
As we’ll see in this article, these software solutions play a pivotal role in modern healthcare settings for several compelling reasons.
Improving Healthcare Efficiency with Software
Efficiency is the lifeblood of any successful healthcare organization. Healthcare software offers numerous opportunities to enhance operational efficiency by simplifying administrative tasks, enabling data-driven decision-making, and ensuring better resource allocation.
Consider the impact of Electronic Health Records, or EHR software. These systems centralize patient information, making it readily accessible to authorized medical personnel. It minimizes the risk of errors while accelerating the decision-making process, leading to faster diagnoses and improved treatment plans.
From a healthcare perspective, this translates to more efficient use of healthcare professionals’ time and improved patient throughput.
Types of Healthcare Software
Now that we’ve established the importance of healthcare software, let’s delve into the various types of healthcare software that significantly impact healthcare organizations and professionals.
Healthcare software can be categorized into several distinct types, each tailored to address specific needs within the healthcare ecosystem. It’s essential to understand these categories and their potential impact on healthcare organizations and professionals:
- Electronic Health Records (EHR) Software: EHR software has revolutionized patient data storage and access. It digitizes patient records, making them easily accessible to authorized medical personnel.
EHR systems enhance the efficiency of healthcare organizations by streamlining record-keeping and improving coordination among healthcare professionals. - Practice Management Software: Healthcare organizations can streamline operations with practice management software. This software helps manage appointments, billing, and administrative tasks efficiently.
Practice management software is valuable for optimizing resource allocation and improving revenue collection. - Telemedicine Software: Telemedicine software has gained immense popularity, especially recently as the Covid-19 pandemic has heavily influenced how people live. It enables remote consultations between patients and healthcare providers, eliminating geographical barriers and expanding access to care. Telemedicine software supports video conferencing, secure messaging, and remote monitoring, allowing for more efficient use of healthcare resources.
Challenges in the Healthcare Industry
The healthcare industry faces many challenges, from rising costs to an aging population and the need for more accessible and affordable care. However, healthcare software offers viable solutions to many of these challenges, aligning with the industry’s goals of improving patient care, reducing costs, and enhancing efficiency.
Let’s look at the challenge of fragmented patient data, for example. In traditional healthcare systems, patient records are often scattered across various providers and facilities, leading to inefficiencies, delayed care, and increased costs. Healthcare software can address this issue by centralizing and standardizing patient records, ensuring that comprehensive and up-to-date information is available when and where it’s needed.
Furthermore, healthcare software can help mitigate the risk of medical errors, which can have profound consequences for you as a patient and even your healthcare provider(s). Decision support systems built into healthcare software provide clinicians with real-time information and clinical guidelines, reducing the likelihood of errors in diagnosis and treatment.
From a healthcare perspective, this translates to improved patient safety and better health outcomes.
Common challenges and risks associated with healthcare software include:
- Data Security: Healthcare software must protect patient data from breaches and cyber threats.
- Interoperability Issues: Incompatibility between systems can hinder data exchange and care coordination.
- Regulatory Compliance: Healthcare software must adhere to stringent regulatory requirements like HIPAA.
- User Resistance: Healthcare professionals may resist adopting new software, affecting its effectiveness.
Managing Cybersecurity Threats
Managing cybersecurity threats is paramount in healthcare software:
- Data Encryption: Encrypt sensitive data at rest and during transmission to prevent unauthorized access.
- Access Controls: Implement strict access controls to limit who can view and modify patient records.
- Regular Audits: Conduct regular security audits and penetration testing to identify vulnerabilities.
- Incident Response Plan: Develop and test an incident response plan to address data breaches promptly.

Regulations and Compliance Standards
Healthcare software must adhere to several regulations and compliance standards:
- HIPAA (Health Insurance Portability and Accountability Act): HIPAA sets standards for protecting patient data privacy and security.
- FDA Regulations: Healthcare software that functions as a medical device must comply with FDA regulations.
- HITECH Act: The Health Information Technology for Economic and Clinical Health (HITECH) Act promotes the adoption of electronic health records and data security.
- GDPR (General Data Protection Regulation): GDPR applies to healthcare organizations that handle data of European Union residents, including patient data.
- Cybersecurity Frameworks: Organizations can follow cybersecurity frameworks such as the NIST (National Institutes of Standards and Technology) Cybersecurity Framework to enhance data protection.
Despite the challenges and risks in using healthcare software, it is possible to efficiently manage these risks.
Benefits of Telemedicine Software for Remote Healthcare Delivery
Telemedicine software is at the forefront of healthcare innovation, offering a means of delivering medical services remotely. Its benefits extend to healthcare providers and patients, making it a transformative tool in the industry.
Here’s how telemedicine software improves remote healthcare delivery:
- Geographical Accessibility: Telemedicine breaks down geographical barriers, allowing patients in rural or underserved areas to access healthcare services without traveling long distances. It’s particularly important for populations with limited access to medical facilities. Telemedicine software has helped in mental health and nutrition counseling, prescribing medicines, and physical therapy.
- Convenience: Patients can schedule virtual appointments at their convenience, reducing wait times and the need for lengthy in-person visits. It’s especially valuable for individuals with busy schedules or mobility challenges. and require non-emergency follow-ups, and tele-intensive care.
- Cost-Efficiency: Telemedicine reduces the costs of in-person visits, such as transportation and childcare expenses. It can also lead to cost savings for healthcare providers by optimizing their use of resources.
- Remote Monitoring: Telemedicine software often includes features for remote patient monitoring. Healthcare providers can track vital signs and chronic conditions, allowing for early intervention and personalized care plans.
- Timely Consultations: In emergencies or situations requiring immediate medical attention, telemedicine provides a platform for quick consultations. It can be critical in cases where time is of the essence.
- Expanded Access to Specialists: Telemedicine enables patients to consult with specialists who may not be available locally. It’s particularly valuable for complex medical conditions that require specialized care.
- Reduced Infection Risk: Especially relevant in times of pandemics and infectious disease outbreaks, telemedicine and minimizes the risk of infection due to contagious illnesses in healthcare settings.
Telemedicine software has rapidly gained popularity, offering a flexible and effective way to deliver healthcare services. Its continued growth is likely to reshape how healthcare is accessed and delivered.
Choosing the Right Healthcare Software
Selecting appropriate healthcare software is a critical decision for healthcare organizations and professionals. Several factors must be considered to ensure the chosen software aligns with the organization’s goals and requirements.

When healthcare organizations and professionals select healthcare software, several factors come into play. These considerations are essential to ensure that the chosen software meets the organization’s needs and objectives:
- Scalability: Healthcare software should be scalable to accommodate the organization’s growth and evolving requirements. It should adapt to changing patient volumes, services, and technology advancements.
- Data Management and Integration: Healthcare generates massive volumes of data, and healthcare organizations are expected to manage its data efficiently, securely, and accurately. Also, healthcare facility use many different systems with unique ways of collecting patient information. Consolidating all the data is often complicated.
- Seamless Billing Processes: Billing is a perennial problem in healthcare; a big headache for both patients and providers. Even with automated billing systems, hospitals may revert to manual intervention to ensure accurate payments. This causes delays in reimbursement, a great inconvenience for patients who need to access funds right away.
- Telehealth Infrastructure: Robust telehealth infrastructure is necessary for access and sharing of health information in a secure, reliable, and quick way. This is the only way to ensure success in a telehealth program.
- Security and Compliance: Robust security measures and compliance with healthcare regulations are non-negotiable. Patient data must be protected, and the software should support compliance with HIPAA and other relevant standards.
Features of Electronic Medical Record (EMR) Software

Electronic Medical Record (EMR) software is a foundational component of healthcare software systems. When evaluating EMR software, healthcare organizations, and professionals should prioritize critical features that support efficient patient care and data management:
- Comprehensive Patient Records: EMR software should enable the creation and maintenance of comprehensive patient records, including medical history, diagnoses, medications, allergies, and treatment plans.
- Integration: EMR systems should seamlessly integrate with other healthcare software and systems to facilitate data exchange and care coordination.
- Decision Support: Decision support tools within EMR software provide real-time guidance to healthcare providers, aiding diagnosis and treatment decisions.
- E-Prescribing: Electronic prescribing capabilities reduce the likelihood of medication errors and support efficient prescription management.
- Clinical Documentation: EMR software should simplify clinical documentation, enabling healthcare providers to record patient encounters and treatment plans efficiently.
- Patient Portal: A patient portal allows patients to access their medical records and test results and communicate with healthcare providers, enhancing patient engagement.
- Reporting and Analytics: EMR software should offer robust reporting and analytics features to support data-driven decision-making and quality improvement initiatives.
Importance of Interoperability
Interoperability is a cornerstone of effective healthcare software systems. It refers to the ability of different software systems, devices, and applications to exchange and use data coherently and coordinated. Interoperability is critical for several reasons:
- Enhanced Care Coordination: Interoperable systems enable healthcare providers to seamlessly access and share patient data. It supports coordinated care and reduces the risk of errors or redundant tests.
- Efficiency: Interoperability reduces the need for manual data entry and paper-based communication, streamlining administrative processes and saving time.
- Patient-Centered Care: Patients benefit from interoperability by having their data accessible across various providers and settings. It ensures continuity of care and reduces the need to repeat medical history.
- Data Accuracy: Automated data exchange minimizes the risk of data entry errors, ensuring healthcare professionals access accurate and up-to-date information.
- Improved Analytics: Interoperable systems enable comprehensive data aggregation and analysis, supporting population health management, research, and quality improvement efforts.
- Cost Savings: Reduced administrative burden and improved efficiency contribute to cost savings for healthcare organizations.
Security and Compliance Considerations
Security and compliance are paramount in healthcare software selection and implementation. Patient data must be protected, and healthcare organizations must adhere to strict regulatory standards. Here are some key considerations:
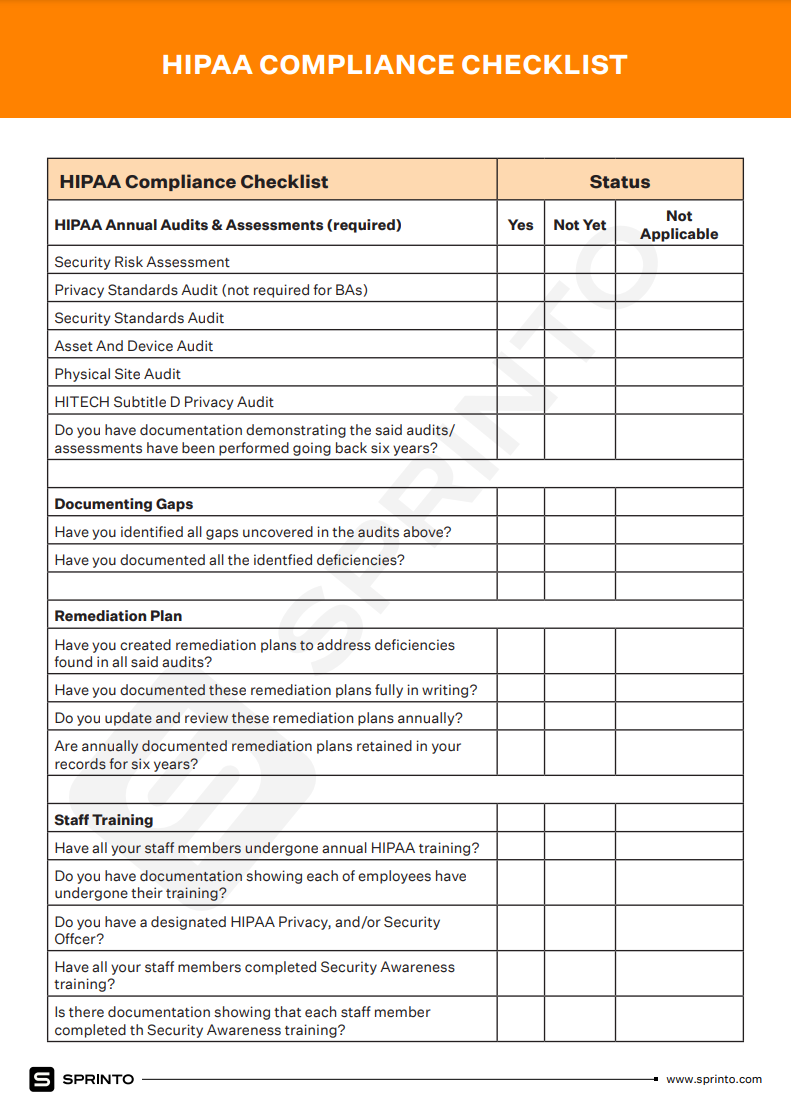
- HIPAA Compliance: Healthcare organizations must ensure software solutions comply with the Health Insurance Portability and Accountability Act (HIPAA) to safeguard patient data.
- Data Encryption: Software should employ robust encryption mechanisms to protect data at rest and during transmission.
- Access Controls: Implement strict access controls to ensure only authorized personnel can access sensitive patient information.
- Regular Auditing: Conduct audits and assessments to identify and address security vulnerabilities.
- Data Backup and Recovery: Implement data backup and recovery processes to ensure data availability in case of emergencies or system failures.
- Training and Awareness: Educate staff about security best practices and safeguarding patient data.
Best Practices for Implementing Healthcare Software
The successful implementation of healthcare software is crucial in realizing its benefits. However, it requires careful planning, collaboration, and adherence to best practices.
To ensure a smooth implementation process, healthcare organizations should consider the following best practices:
- Needs Assessment: Conduct a comprehensive needs assessment to identify the specific requirements and goals of the organization.
- Stakeholder Engagement: Involve all relevant stakeholders, including healthcare professionals, administrators, and IT personnel, in the decision-making process.
- Clear Objectives: Define clear objectives and expected outcomes for the implementation.
- Project Management: Appoint a project manager or team to oversee the implementation process, ensuring that timelines and budgets are followed.
- Training: Provide thorough training to staff members who will use the software. Ensure that they’re proficient in its use before full implementation.
- Testing and Quality Assurance: Thoroughly test the software to identify and address any issues or bugs before full deployment.
- Change Management: Implement change management strategies to help staff adapt to new processes and workflows.
- Data Migration: Plan and execute data migration carefully to ensure that existing patient data is transferred accurately.
Ensuring Smooth Integration of Healthcare Systems

Integration with existing systems is often a complex aspect of healthcare software implementation. To ensure smooth integration, organizations should have:
- Compatibility Assessment: Determine the compatibility of the new software with existing systems and identify any potential integration challenges.
- Interoperability Standards: Ensure the software meets interoperability standards to facilitate seamless data exchange.
- API Integration: Utilize Application Programming Interfaces (APIs) to connect and exchange data between systems.
- Data Mapping: Map the data fields and structures between systems to ensure accurate data transfer.
- Testing: Rigorously test integration points to identify and resolve any issues.
- Data Validation: Validate data during integration to ensure accuracy and completeness.
- Continuous Monitoring: Implement continuous monitoring to identify and address integration issues as they arise.
Common Challenges in Healthcare Software Implementation
While the benefits of healthcare software implementation are substantial, challenges can arise during the process. Common challenges include:
- Resistance to Change: Healthcare professionals may resist changes to established workflows and processes.
- Technical Issues: Technical glitches or compatibility problems can disrupt implementation.
- Data Migration Errors: Errors in data migration can result in data loss or inaccuracies.
- Training Gaps: Insufficient training can lead to user errors and reduced software adoption.
- Integration Complexity: Complex integrations with existing systems may require significant resources.
Working with a qualified healthcare systems company like Iterators helps to anticipate and navigate these challenges easily, quickly, and cost-effectively.
Facilitating Training and User Adoption for Healthcare Software

Effective training and user adoption are essential for realizing the benefits of healthcare software. To facilitate training and adoption:
- Comprehensive Training: Provide thorough user training tailored to their roles and responsibilities.
- User Support: Offer ongoing user support and resources, such as help desks or tutorials.
- Feedback Mechanisms: Encourage user feedback to identify areas for improvement and address concerns.
- Champion Users: Identify and leverage “champion users” who can advocate for the software and assist colleagues.
- Continuous Training: Implement training programs to update users on software enhancements and best practices.
Impact of Healthcare Software on Patient Care
The adoption of healthcare software has a profound impact on patient care, spanning improved engagement, clinical decision-making, predictive analytics, and enhanced outcomes.
Enhancing Patient Engagement and Satisfaction with Healthcare Software
Patient engagement is a crucial aspect of healthcare, and healthcare software plays a pivotal role in enhancing patient satisfaction and involvement in their care. Here are some benefits of using healthcare software in patient management:
- Access to Information: Patients can access their health records, test results, and treatment plans through patient portals, empowering them with information and fostering engagement in their healthcare decisions.
- Convenient Communication: Secure messaging and telehealth features enable patients to communicate with healthcare providers conveniently, reducing barriers to seeking premium and effective care.
- Appointment Scheduling: Online appointment scheduling and reminders improve convenience and help patients stay engaged with their care.
- Medication Management: Medication reminders and electronic prescription refills enhance medication adherence.
- Health Education: Healthcare software often includes educational resources and personalized health information, supporting patient understanding and self-management.
- Feedback Mechanisms: Patients can provide feedback on their experiences, helping healthcare organizations continually improve care quality.
Improving Clinical Decision-Making with Software Solutions
Clinical decision-making benefits significantly from healthcare software, with several key advantages:
- Access to Comprehensive Data: Electronic health records provide a complete patient history, supporting accurate diagnoses and treatment decisions.
- Decision Support Tools: Built-in decision support tools offer real-time guidance based on best practices and clinical guidelines.
- Data Analytics: Software solutions enable data analysis, identifying trends and outcomes that inform clinical decisions.
- Interoperability: Interoperable systems provide access to external data sources, such as lab results or radiology reports, enhancing clinical insight.
- Risk Assessment: Predictive analytics can identify patients at risk of specific conditions or adverse events, allowing for proactive intervention.
Using Predictive Analytics and Machine Learning Algorithms to Improve Healthcare Outcomes
Predictive analytics and machine learning algorithms are game-changers in healthcare, offering the potential to enhance outcomes through:
- Risk Stratification: Identifying patients at higher risk of diseases or complications enables early intervention and preventive measures.
- Resource Allocation: Predictive analytics help healthcare organizations allocate resources efficiently, such as hospital beds and staff, based on anticipated patient needs.
- Personalized Medicine: Machine learning models can analyze patient data to recommend personalized treatment plans and interventions.
- Disease Detection: Algorithms can detect subtle patterns in medical data, aiding in the early detection of diseases or conditions.
- Population Health Management: Predictive analytics support population health initiatives by identifying trends and areas for improvement in patient populations.
Case Studies
Real-world case studies demonstrate the tangible impact of healthcare software on patient care and healthcare organizations. Here are a few examples:
- Improved Chronic Disease Management: A healthcare system, Patient Care Medical Home (PCMH), in Vermont, USA, implemented patient monitoring software, significantly reducing hospital readmissions and total healthcare costs for patients with chronic conditions.
- Enhanced Care Coordination: An integrated EHR system reduced duplicate testing and improved care coordination among specialists, leading to better patient outcomes in low-income countries.
- Telemedicine’s Reach: A rural healthcare clinic expanded its services through telemedicine, increasing access to care for underserved populations.
- Predictive Analytics in Action: A hospital system used predictive analytics to identify patients at high risk of sepsis, resulting in superior outcomes in mental health cases.
- Patient Engagement: A patient portal and mobile app improved patient engagement, with more patients actively using these tools to manage their health. Iterators are especially suited to reshape your healthcare business through electronic patient engagement.
- Personalized Treatment: The e-health company eCuris built a platform whose machine-learning algorithms identify the most effective treatments for patients, help doctors track patients, and help patients monitor their health. US hospitals also improve the management of patients with chronic conditions and use social networks to engage, inform, and educate patients on their health.
It has resulted in higher health recovery rates and improved quality of life. - Resource Optimization: Predictive analytics optimized hospital bed utilization, reducing wait times and enhancing patient flow in a New York hospital that overhauled its Standard Operating Procedures (SOPs) using healthcare software.
Future Trends and Innovations in Healthcare Software

The future of healthcare software is brimming with promise, driven by emerging technologies, artificial intelligence (AI), automation, and a commitment to solving complex healthcare challenges.
Several emerging technologies are poised to shape the future of healthcare software:
- Artificial Intelligence (AI): Artificial intelligence enables healthcare systems to make decisions with minimal human input by continuously learning patterns. AI-powered algorithms and machine learning models will continue to advance, supporting diagnostic accuracy, predictive analytics, and personalized treatment plans.
- Internet of Things (IoT): IoT devices and sensors will play an increasingly significant role in data collection, enabling real-time monitoring and early intervention. IoT enables devices to interact in real time.
- Blockchain: Blockchain technology will enhance data security, streamline data sharing, and improve the integrity of healthcare records. Blockchain systems promote transparency and security.
- Augmented and Virtual Reality (AR/VR): AR and VR applications will be used for medical training, patient education, and even remote surgical procedures These technologies allow for a more comprehensive diagnosis and prognosis of health conditions
- Genomics: Genomic data integration will enable personalized medicine, with treatment plans tailored to an individual’s genetic makeup.
- Chatbots and Virtual Assistants: AI-driven chatbots and virtual assistants will respond immediately to patient queries, schedule appointments, and offer medication reminders. These virtual beings are similar to unmanned vehicles and spacecraft, bringing autonomy to the healthcare space.
- 5G Connectivity: 5G networks are a significant upgrade to current 4G connections and will have an important impact on broadband internet, including enabling faster data transmission and supporting real-time telehealth applications.
Using AI and Automation to Improve Healthcare Processes
AI and automation are poised to revolutionize healthcare processes in several ways:
- Predictive Analytics: AI-driven predictive analytics will identify disease trends and population health risks, enabling proactive interventions.
- Robotic Process Automation (RPA): RPA will automate administrative tasks, reducing the burden on healthcare staff and improving efficiency.
- Natural Language Processing (NLP): NLP will enhance clinical documentation and support voice-enabled interfaces for healthcare providers.
- Drug Discovery: AI algorithms will accelerate drug discovery and development, leading to more effective treatments.
- Personalized Treatment Plans: AI will analyze patient data to recommend personalized treatment plans, minimizing trial-and-error approaches.
- Remote Monitoring: AI-powered remote monitoring will detect early signs of deterioration in patients, enabling timely interventions.
- Clinical Decision Support: AI-based clinical decision support systems will provide real-time guidance to healthcare providers based on the latest research and best practices.
Blockchain Technology and Healthcare Data Security
Blockchain technology holds significant potential for healthcare data security:
- Immutable Records: Blockchain creates immutable and tamper-proof records, ensuring the integrity of patient data.
- Data Sharing: Patients can control access to their data through blockchain-based consent management, enhancing privacy.
- Interoperability: Blockchain can facilitate secure data exchange between different healthcare systems, supporting care coordination.
- Clinical Trials: Blockchain can streamline clinical trial data management, improving transparency and accountability.
- Supply Chain Management: Blockchain can enhance the traceability and security of pharmaceutical supply chains, reducing the risk of counterfeit drugs.
Ethical and Privacy Concerns in Advanced Healthcare Software
As healthcare software advances, ethical and privacy concerns must be addressed:
- Data Privacy: Protecting patient data and ensuring informed consent for data use are essential.
- Bias in AI Algorithms: AI algorithms must be carefully designed to avoid biases that could lead to healthcare disparities.
- Security Vulnerabilities: Robust security measures are needed to protect against cyber threats and data breaches.
- Informed Decision-Making: Healthcare providers and patients must clearly understand how AI and data analytics influence clinical decisions.
Integrating Healthcare Software with the Internet of Things (IoT)
Integrating healthcare software with IoT devices and sensors opens new frontiers in data collection, analysis, and care delivery. The Internet of Things refers to the network of connected devices that enables communication between devices and the cloud, and between the said devices.
Integrating IoT Devices and Sensors into Healthcare Software
Effective integration of IoT devices and sensors into healthcare software involves:
- Device Compatibility: Ensure IoT devices are compatible with the software and can transmit data seamlessly.
- Data Standards: Establish standardized protocols for data transmission and device communication.
- Data Security: Implement robust security measures to protect IoT data, which can be sensitive and personal.
- Real-Time Monitoring: Use IoT data for real-time patient monitoring, enabling timely interventions.
- Data Analytics: Leverage IoT-generated data for predictive analytics and population health management.
Benefits of Leveraging IoT in Healthcare for Data Collection and Analysis
The benefits of IoT in healthcare software include:
- Remote Monitoring: IoT devices enable remote patient monitoring, reducing hospital readmissions and enhancing chronic disease management.
- Early Intervention: Real-time data from IoT sensors can trigger alerts for healthcare providers, allowing for early intervention in critical situations.
- Personalized Care: IoT data facilitates personalized treatment plans tailored to an individual’s health metrics.
- Research and Population Health: Aggregated IoT data supports medical research and population health management by identifying trends and patterns.
- Enhanced Patient Engagement: Patients become more engaged in their healthcare when they can access real-time data and insights.
Use Cases of IoT in Healthcare Software
Integrating healthcare software with IoT devices and sensors opens new data collection, analysis, and care delivery possibilities. It supports remote monitoring, early intervention, and personalized care plans. IoT is already making a significant impact on healthcare, with various use cases, including:
- Wearable Devices: Smartwatches and fitness trackers collect data on physical activity, heart rate, and sleep patterns.
- Remote Monitoring: IoT-enabled devices can monitor vital signs, glucose levels, and medication adherence in real time.
- Smart Home Healthcare: IoT devices in a patient’s home can monitor their environment and health, providing necessary alerts and assistance.
- Asset Tracking: Hospitals use IoT to track the location and status of medical equipment, optimizing resource allocation.
- Environmental Monitoring: IoT sensors can monitor air quality and temperature in healthcare facilities to ensure a safe and comfortable environment.
The Takeaway
In the ever-evolving landscape of healthcare, software solutions are catalysts for change. From electronic health records (EHR) software that centralizes patient information to telemedicine software that expands access to care, healthcare software can transform the industry.
Choosing the right healthcare software involves considering scalability, interoperability, user-friendliness, customization, and robust security. Implementing best practices, including needs assessment, stakeholder engagement, and comprehensive training, is vital for success.
The impact of healthcare software on patient care is profound, from improved engagement and clinical decision-making to the use of predictive analytics and machine learning. There are tangible benefits of healthcare software for patients and healthcare organizations.
The future of healthcare software is bright, driven by emerging technologies like AI, IoT, and blockchain. These technologies promise to enhance data security, automation, and personalized care. However, they also bring ethical and privacy concerns that must be addressed. Considering its robust track record, Iterators is the preferred partner for individuals and organizations building innovative healthcare solutions.
In conclusion, healthcare software isn’t just a tool; it’s a transformative force that can improve patient care, streamline operations, and drive innovation in the healthcare industry. Contact Iterators to embrace the potential of healthcare software is a strategic choice and a commitment to delivering better, more accessible, and efficient healthcare for all.

